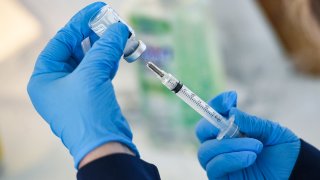
Many Americans who received the Pfizer COVID vaccine are now eligible for booster doses, but what about those who received the Moderna or Johnson & Johnson vaccines?
Here's what we know so far:
Can I get a booster shot now?
Some people who received the Moderna vaccine are already eligible for booster shots, but for those who received Johnson & Johnson, a decision has not yet been made.
Get Boston local news, weather forecasts, lifestyle and entertainment stories to your inbox. Sign up for NBC Boston’s newsletters.
U.S. regulators are expected to decide at a later date on widespread boosters for those brands. The government also said it has no data on whether it is safe or effective to mix-and-match and give those people a Pfizer shot.
Adding to the complexity of further decisions on booster shots, Moderna wants its third dose to be half of the original shots.
Moderna previously released data on breakthrough cases, saying it supports the push for wide use of COVID-19 vaccine booster shots.
Local
In-depth news coverage of the Greater Boston Area.
But as the FDA's Vaccines and Related Biological Products Advisory Committee debated administering third doses of Pfizer and BioNTech's vaccine, federal health regulators said they needed more time to review Moderna's application for extra doses.
The U.S. has, however, already approved both Pfizer and Moderna boosters for certain people with weakened immune systems, such as cancer patients and transplant recipients.
According to the CDC, the list includes people who have:
- Been receiving active cancer treatment for tumors or cancers of the blood
- Received an organ transplant and are taking medicine to suppress the immune system
- Received a stem cell transplant within the last 2 years or are taking medicine to suppress the immune system
- Moderate or severe primary immunodeficiency (such as DiGeorge syndrome, Wiskott-Aldrich syndrome)
- Advanced or untreated HIV infection
- Active treatment with high-dose corticosteroids or other drugs that may suppress your immune response
The agency notes that "people should talk to their healthcare provider about their medical condition, and whether getting an additional dose is appropriate for them."
The FDA and CDC’s approval and recommendation for immunocompromised individuals does not apply to those who got the Johnson & Johnson vaccine.
Johnson & Johnson released data last week showing that a booster dose to its one-shot coronavirus vaccine provides a strong immune response months after people receive a first dose.
J&J said in statement that it ran two early studies in people previously given its vaccine and found that a second dose produced an increased antibody response in adults from age 18 to 55. The study's results haven't yet been peer-reviewed.
The company is in talks with regulators including the U.S. Food and Drug Administration, the European Medicines Agency and others regarding using booster doses of its vaccine.
Health officials have said they were expecting to receive more data in the fall and will "keep the public informed with a timely plan for J&J booster shots as well."
Who is eligible now under the recent guidance?
Under the CDC's endorsement, boosters should be offered to people 65 and older, nursing home residents and those ages 50 to 64 who have risky underlying health problems.
CDC Director Dr. Rochelle Walensky, however, added to that list people ages 18 to 64 years who are health-care workers or have another job that puts them at increased risk of being exposed to the virus.
The FDA had already authorized booster doses for Americans who are 65 and older, younger adults with underlying health conditions and those in jobs that put them at high risk for COVID-19.
The extra dose would be given once they are at least six months past their last Pfizer shot. Those who received Moderna or Johnson & Johnson vaccines are not yet eligible.
Here's the latest list of who qualifies, according to the CDC:
- People 65 years and older and residents in long-term care settings should receive a booster shot of Pfizer-BioNTech’s COVID-19 vaccine at least 6 months after their Pfizer-BioNTech primary series,
- People aged 50–64 years with underlying medical conditions should receive a booster shot of Pfizer-BioNTech’s COVID-19 vaccine atleast 6 months after their Pfizer-BioNTech primary series,
- People aged 18–49 years with underlying medical conditions may receive a booster shot of Pfizer-BioNTech’s COVID-19 vaccine at least 6 months after their Pfizer-BioNTech primary series, based on their individual benefits and risks, and
- People aged 18-64 years who are at increased risk for COVID-19 exposure and transmission because of occupational or institutional setting may receive a booster shot of Pfizer-BioNTech’s COVID-19 vaccine at least 6 months after their Pfizer-BioNTech primary series, based on their individual benefits and risks.
What counts as a qualifying underlying health condition? Here's a list from the CDC:
- Cancer
- Chronic kidney disease
- Chronic lung diseases, including COPD, asthma (moderate-to-severe), interstitial lung disease, cystic fibrosis, and pulmonary hypertension
- Dementia or other neurological conditions
- Diabetes (type 1 or type 2)
- Down syndrome
- Heart conditions (such as heart failure, coronary artery disease, cardiomyopathies or hypertension)
- HIV infection
- Immunocompromised state (weakened immune system)
- Liver disease
- Overweight and obesity
- Pregnancy
- Sickle cell disease or thalassemia
- Smoking, current or former
- Solid organ or blood stem cell transplant
- Stroke or cerebrovascular disease, which affects blood flow to the brain
- Substance use disorders
President Joe Biden on Friday urged those who are now eligible to get a booster shot.
"My message today is this: If you've got the Pfizer vaccine, you got the Pfizer vaccine in January, February, or March of this year, and you're over 65 years of age, go get the booster," he said. "Or if you have a medical condition like diabetes, or you're a frontline worker like a health care worker or teacher, you can get a free booster now."
When might I be able to get a booster shot?
Despite the resistance in recent days, some top U.S. health officials said they expect boosters to eventually win broader approval in the coming weeks or months. Dr. Anthony Fauci said over the weekend that “this is not the end of the story.”
The CDC panel stressed that its recommendations will be changed if new evidence shows more people need a booster.
Further timing remains unclear.
If I got the Moderna or J&J vaccine, should I get a booster shot of the Pfizer vaccine?
Federal experts have indicated the Pfizer shots would not be recommended for people who got a different brand of vaccine initially.
"That's a question that's been looked at to some extent in the U.K.," Boston Medical Center's Dr. Davidson Hamer told NBC10 Boston last week. "AstraZeneca was followed by Pfizer and has shown fairly robust immune response. The vaccine works in slightly different ways. We need more evidence, although the initial evidence shows that approach is safe."
For those who received the Moderna or Pfizer vaccine, the CDC says "a third dose of the same mRNA vaccine should be used."
"A person should not receive more than three mRNA vaccine doses. If the mRNA vaccine product given for the first two doses is not available or is unknown, either mRNA COVID-19 vaccine product may be administered," the agency's website states.
When can eligible people get their third dose?
For those eligible under the recent rulings from the FDA and CDC, the extra dose would be given once they are at least six months past their last Pfizer shot.
The FDA determined that transplant recipients and others with a similar level of compromised immunity can receive a third dose of the vaccines from Pfizer and Moderna at least 28 days after getting their second shot.
Walgreens announced last month that its pharmacies will offer additional COVID-19 vaccine doses to eligible patients with compromised immune systems.
Walgreens has begun offering same-day appointments available to such patients on a walk-in basis at select stores, the company said. Patients will bring their vaccination card or record to the appointments to prove eligibility.
Under the recent FDA authorization for seniors and high-risk populations, eligible vaccinated Americans would be able to receive their third dose six months after receiving their second Pfizer shot.
Are there any risks with getting a booster shot? What about side effects?
Among people who stand to benefit from a booster, there are few risks, the CDC concluded. Serious side effects from the first two Pfizer doses are exceedingly rare, including heart inflammation that sometimes occurs in younger men. Data from Israel, which has given nearly 3 million people — mostly 60 and older — a third Pfizer dose, has uncovered no red flags.
The CDC has noted that side effects with the third shot "were similar to that of the two-dose series."
The most common symptoms include fatigue and pain at the injection site, but "most symptoms were mild to moderate."
As with previous doses of the vaccine, the CDC notes that, "serious side effects are rare, but may occur."
Will booster shots contain the original vaccine, or one tailored to delta?
The boosters will be an extra dose of the original vaccine. Manufacturers still are studying experimental doses tweaked to better match delta. There’s no public data yet that it’s time to make such a dramatic switch, which would take more time to roll out. And independent research shows the original vaccine produces antibodies that can target delta.
“I’m very, very confident that this vaccine will work against delta with a single booster of the same vaccine,” Pfizer CEO Albert Bourla told The Associated Press.
How much protection will I get?
No one yet knows “the magic line” — the antibody level known as the correlate of protection below which people are at risk for even mild infection, experts say. But vaccines’ main purpose is to prevent severe disease.
Plus, people’s responses to their initial vaccination vary. Younger people, for example, tend to produce more antibodies to begin with than older adults. That means months later when antibody levels have naturally declined, some people may still have enough to fend off infection while others don’t.
CDC data shows the vaccines still offer strong protection against serious illness for all ages, but there is a slight drop among the oldest adults. And immunity against milder infection appears to be waning months after people's initial immunization.
Won't antibodies wane again even after a booster?
Eventually. “We don’t know the duration of protection following the boosters,” cautioned Dr. William Moss of Johns Hopkins University.
But antibodies are only one defense. If an infection sneaks past, white blood cells called T cells help prevent serious illness by killing virus-infected cells. Another type called memory B cells jump into action to make lots of new antibodies.
Those back-up systems help explain why protection against severe COVID-19 is holding strong so far for most people. One hint of trouble: CDC has preliminary data that effectiveness against hospitalization in people 75 and older dropped slightly in July -- to 80% -- compared to 94% or higher for other adults.
Am I still considered fully vaccinated if I don't get a booster?
Even with the introduction of boosters, someone who has gotten just the first two doses would still be considered fully vaccinated, according to the CDC's Dr. Kathleen Dooling. That is an important question to people in parts of the country where you need to show proof of vaccination to eat in a restaurant or enter other places of business.



