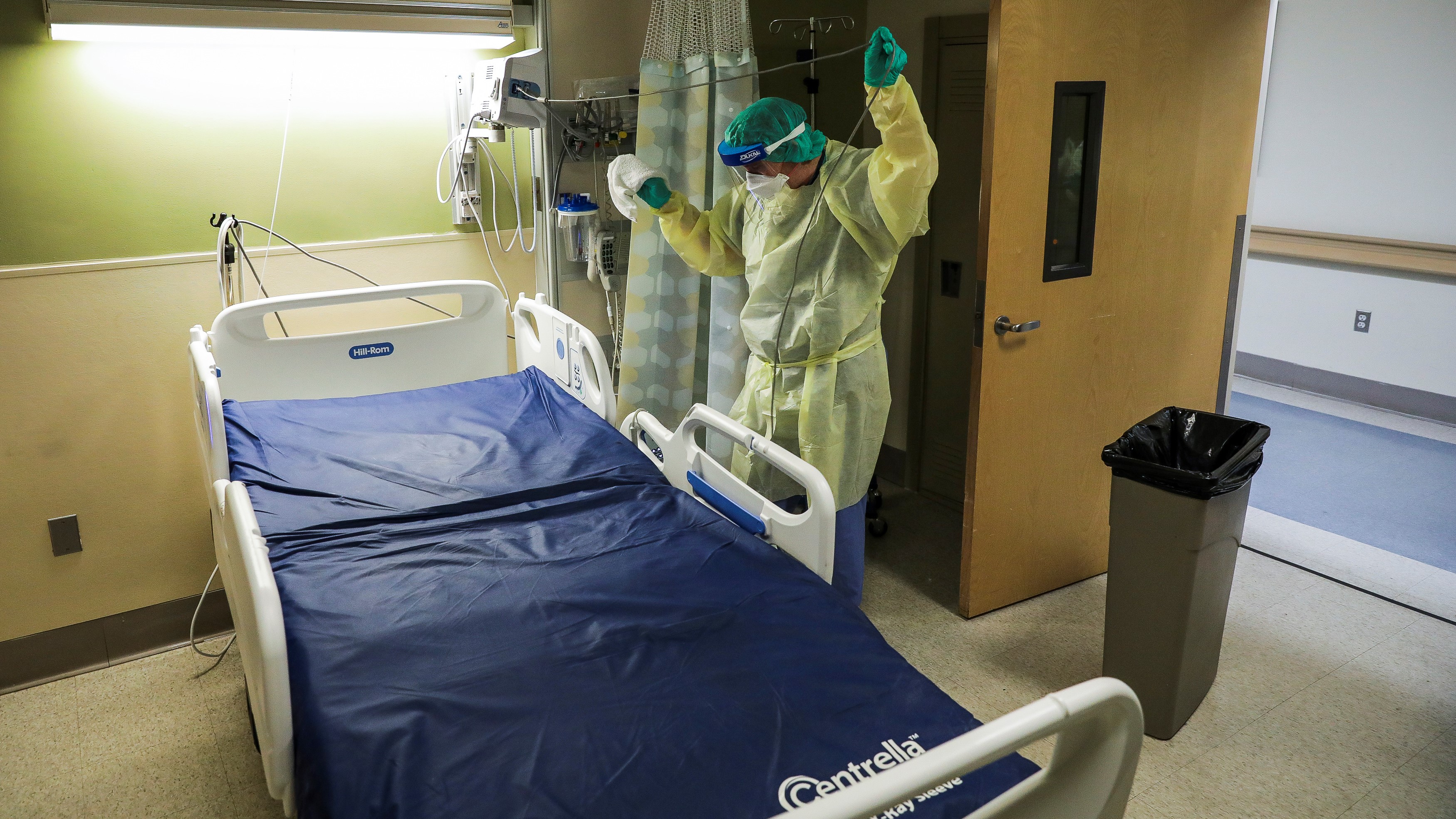
Experts are predicting a winter surge in coronavirus cases -- particularly after more people get together to celebrate the holiday season.
In fact, COVID hospitalizations are already on the rise. Massachusetts health officials on Wednesday reported the highest number of hospitalized patients since the beginning of March.
Meanwhile, hospitals across the state are struggle with bed and staffing shortages, an issue that prompted the Baker administration to order hospitals with bed shortages to cease non-urgent procedures effective Nov. 29.
As part of the weekly series, "COVID Q&A," NBC10 Boston asked three top Boston doctors on Tuesday to explain what symptoms people should watch out for after holiday gatherings and how to differentiate coronavirus from the common cold.
Get Boston local news, weather forecasts, lifestyle and entertainment stories to your inbox. Sign up for NBC Boston’s newsletters.
What are COVID symptoms?
A cough, sore throat, loss of smell and taste -- these are some of the symptoms most commonly associated with the coronavirus. But people with COVID-19 have had a wide range of symptoms, ranging from mild to severe.
Symptoms can show up anywhere from two to 14 days after someone has been exposed to the virus. According to the U.S. Centers for Disease Control and Prevention, people with the following symptoms may have COVID-19:
- Fever or chills
- Cough
- Shortness of breath or difficulty breathing
- Fatigue
- Muscle or body aches
- Headache
- New loss of taste or smell
- Sore throat
- Congestion or runny nose
- Nausea or vomiting
- Diarrhea
So-called COVID-19 “long-haulers" sometimes experience neurological symptoms, which can also be mild to severe. Those symptoms can include headaches, dizziness, numbness and tingling in the extremities and altered brain function, studies have shown.
Another condition, dubbed "COVID toes," can develop, as well as other rashes. These skin manifestations may arise due to clotting in smaller blood vessels, Hamer explained. Therefore, they may have a similar path to symptoms as some of the neurological complications, particularly stroke.
A symptom often described by patients as "brain fog," has been reported among people who experience difficulty concentrating and remembering things.
Is it COVID or the common cold?
Boston doctors say it is very difficult to differentiate between COVID and the common cold because the symptoms can be so similar.
"If you lose your sense of smell and taste that's almost certainly COVID-19," Dr. Shira Doron of Tufts Medical Center said. "I have heard people get confused because when you have a very stuffy nose, obviously your smell and taste are diminished. That's different. You know, it's a real neurologic loss of smell and taste that you get with COVID-19 and if you have that, that's pretty much always COVID-19. But other than that, they can look like any other virus."
"Basically any minor symptom might be COVID-19," Boston Medical Center's Dr. David Hamer added, "especially in the context of somebody who's been previously vaccinated or a younger, healthy adult or child because they may have very mild symptoms."
When experiencing symptoms, experts say it's best to play it safe by isolating and getting tested.
"My feeling is that even the slightest symptom of a cold means you should get tested. It is never wrong to be tested," Doron said. "But any symptom, a new runny nose, stuffy nose, a new sore throat -- even mild -- especially in the era of vaccination, that can be your manifestation of COVID-19."
Doron recommends getting a PCR test over an antigen test. Home kits, which rely on antigen testing, are not as accurate as the PCR tests done in hospitals and at testing sites, but they have the advantage of giving results within minutes instead of days.
"If you get a PCR test and it's negative, then you know, even if the symptoms get a little worse, that's okay," Doron said. "If you are symptomatic and it's the beginning of symptoms and you get an antigen test well, you know, that you may want to repeat again the next day and the next day to be sure."
Home tests will miss some infections and in rare cases mistakenly indicate an infection. One popular test misses around 15 out of 100 infections — these are called “false negatives” — and gives a false positive result in about 1 in 100 people who aren’t infected.
Hamer recommends that people take extra precautions in the seven to 10 days after attending an event with a large group of people.
"You're not quarantine, but be very cautious with with others that you have contact with them, you know, where possible," Hamer said. "If you're in public places, wear masks because there's a possibility that you could have been exposed and might be incubating and that you can then pass on the virus."
More from the COVID Q&A series
A panel of Boston-based doctors talking about everything related to the COVID-19 pandemic.