The World Health Organization could decide as soon as Friday whether or not to declare monkeypox a global health emergency.
A public health emergency of international concern is the organization’s highest alert. This decision will come after intense scrutiny over how they first handled the COVID-19 pandemic in 2020
If monkeypox is declared a global health emergency, that could escalate a world-wide response, especially as cases rise sharply in Britain. They’ve had almost 800 cases reported there, within the past month – a nearly 40% increase in a 5-day span.
It’s been an ongoing crisis in Africa for years.
Get Boston local news, weather forecasts, lifestyle and entertainment stories to your inbox. Sign up for NBC Boston’s newsletters.
Here in Massachusetts, the state Department of Public Health just announced six additional cases of monkeypox in adult men within the past week. They’re currently in isolation while contract tracing efforts are underway.
The total number of cases is now up to 13 statewide, since it was first detected here about five weeks ago on May 18. Only one other case has been confirmed elsewhere in New England so far, in a Rhode Island resident who had recently traveled to Massachusetts.
There have not been any deaths related to the monkeypox outbreak and patients generally recover within about two to four weeks.
In New York, where 30 cases have now been identified, health officials began administering the monkeypox vaccine this week.
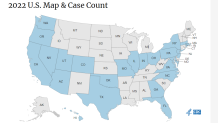
As of Thursday, there were a total of 173 confirmed monkeypox cases in the U.S., according to the Centers for Disease Control and Prevention. Over 3,500 cases have been confirmed worldwide.
How do you catch monkeypox?
The CDC issued new monkeypox guidance last week as the number of suspected cases nationwide boomed, marking America's largest-ever outbreak of monkeypox, which typically has been confined to other continents.
While the CDC says the risk to the general public remains low, people are urged to avoid close contact with those who are sick, including those with skin or genital lesions, as well as sick or dead animals. Anyone displaying symptoms, like unexplained skin rash or lesions, should reach out to their healthcare providers for guidance.
What you should do if you think you might have monkeypox
Anyone with a rash that looks like monkeypox should talk to their healthcare provider, even if they don’t think they had contact with someone who has monkeypox. According to the CDC, people who may be at higher risk might include but are not limited to those who:
- Had contact with someone who had a rash that looks like monkeypox or someone who was diagnosed with confirmed or probable monkeypox
- Had skin-to-skin contact with someone in a social network experiencing monkeypox activity, this includes men who have sex with men who meet partners through an online website, app or social event
- Traveled outside the U.S. to a country with confirmed cases of monkeypox or where monkeypox activity has been ongoing
- Had contact with a dead or live wild animal or exotic pet that exists only in Africa or used a product derived from such animals (e.g., game meat, creams, lotions, powders, etc.)
How did monkeypox start? What is it?
Monkeypox was first discovered in 1958, when outbreaks occurred in colonies of monkeys kept for research -- resulting in its name.
The first case in a human was reported in 1970 in the Democratic Republic of the Congo, which still has the majority of infections. Other African countries where it has been found: Cameroon, Central African Republic, Cote d’Ivoire, Democratic Republic of the Congo, Gabon, Liberia, Nigeria, Republic of the Congo and Sierra Leone.
What are the symptoms of monkeypox?
Human symptoms of monkeypox are similar to but milder than the symptoms of smallpox, the CDC says. It presents itself as a flu-like illness accompanied by lymph-node swelling and rash on the face and body.
Monkeypox starts off with fever, headache, muscle aches, and exhaustion. Monkeypox also causes lymph nodes to swell, something that smallpox does not. The incubation period is usually 7 to 14 days but can range from 5 to 21 days.
The CDC is urging healthcare providers in the U.S. to be alert for patients who have rashes consistent with monkeypox, regardless of whether they have traveled or have specific risks for monkeypox. See more information from the travel notice here.



