The number of patients who are severely ill with COVID-19 is less than half of all those hospitalized with the virus, Boston doctors said Tuesday, but that doesn't mean there's any less strain on the health care system.
Hospitals have started to differentiate between patients they admit primarily for severe COVID-19 and those admitted to be treated for something else who end up testing positive. The change in reporting cut the number of what had been reported as COVID-19 hospitalizations in half.
The idea is to give the public a better understanding of how many people are in the hospital because of the virus. But while that data began to be collected last week, it won't be released by the Massachusetts Department of Public Health until sometime this week.
During NBC10 Boston's weekly "COVID Q&A" series Tuesday, Tufts Medical Center's hospital epidemiologist Dr. Shira Doron said in a week's worth of data, the number of patients being treated for severe COVID-19 was considerably below 50% of all COVID-19 hospitalizations.
Get Boston local news, weather forecasts, lifestyle and entertainment stories to your inbox. Sign up for NBC Boston’s newsletters.
She specified that under the new guidelines, hospitals are reporting the proportion of patients who received the drug Dexamethasone, a steroid used to reduce inflammation, at some point during their hospitalization vs. those who are COVID positive and in the hospital.
"One day was as low as 36%," Doron said of the data. "The state actually called and said, 'Are you sure that it's only 36%?' And so we took a look and indeed, none of those patients were receiving any supplemental oxygen."
The data indicates that although patients may have been in the hospital with COVID-19, the majority of them didn't need any oxygen, she explained. And Tufts Medical Center isn't the only hospital reporting lower numbers.
"We looked at what the other hospitals were reporting that day and we found that we weren't an outlier in that," Doron said. "And so I think that, you know, from Massachusetts, where again, we do mandatory testing of everybody on admission, we may find relatively lower than expected, I think, proportions of patients receiving that drug, which is the standard of care."
Dr. Daniel Kuritzkes, chief of infectious disease at Brigham and Women's Hospital, said his experience was "exactly the same," as Doron's.
"Most of the patients from I was seeing who happened to test positive for COVID were there for another reason and had very mild COVID or had already recovered but were still positive," he said.
Despite the fact that the number of patients with severe COVID-19 is far less than what was being reported previously, hospitals continue to struggle. COVID-19 hospitalizations have surged over the last month as the omicron variant has become dominant. Meanwhile, hospitals are dealing with staffing shortages that are further stressing the system and limiting bed capacity.
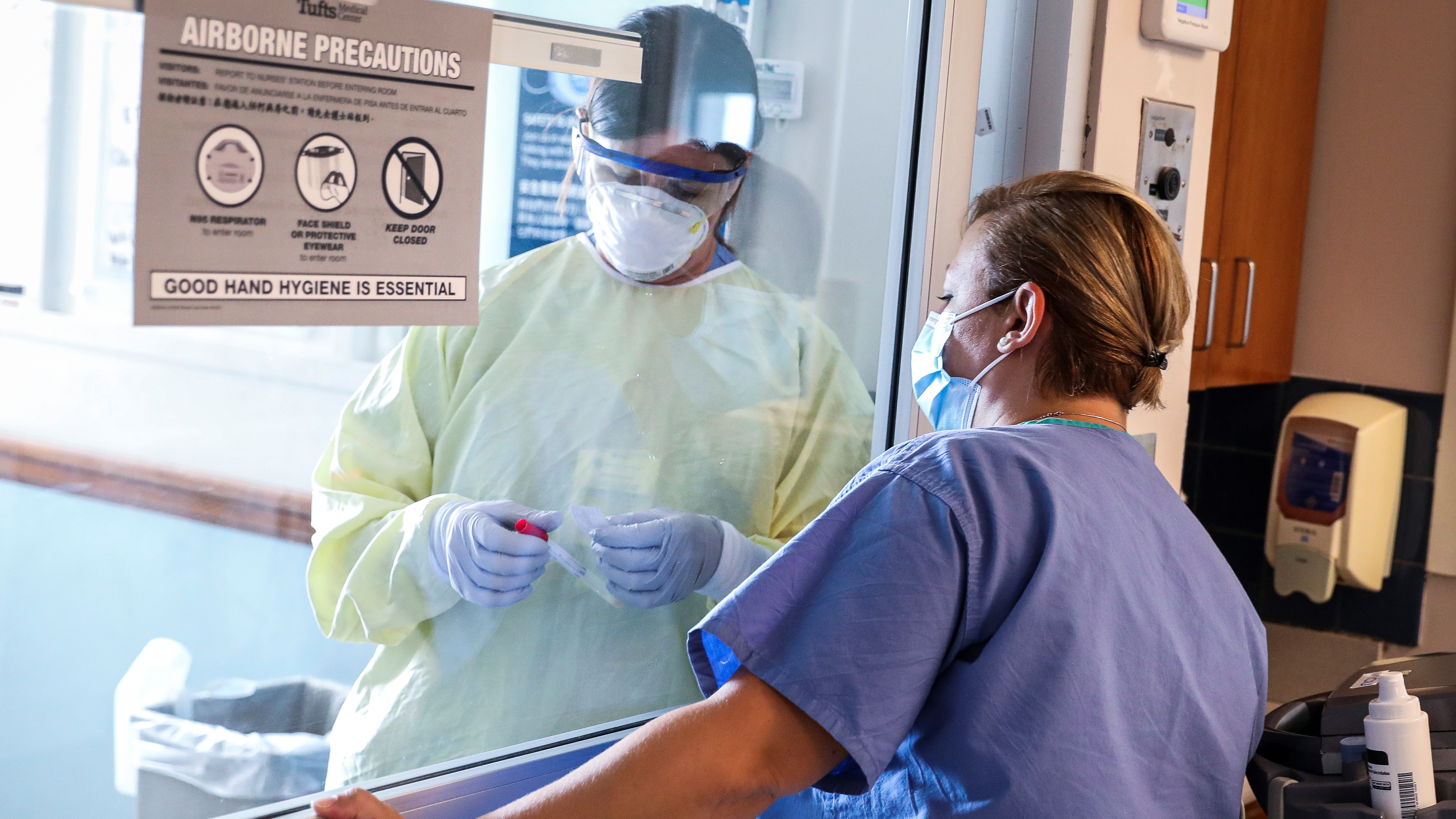
Health care providers still need the gown, glove and N95 masks to go in and see those patients, along with other safety protocols, even if they aren't severely ill.
"The problem for the hospitals is that those patients cause just as much inconvenience and disruption to normal hospital services because they still all need to be in a single, isolation room or cohorted with another COVID person," Kuritzkes said. "So despite the fact that it's good to see fewer people requiring care for their COVID, it's enormously disruptive and having a huge impact on provision of services in the hospital."